Recent Posts
How to Tell If “Just Tired” Might Be Something More

Everyone feels tired sometimes. Long workdays, busy schedules, poor sleep and stress can all leave you drained. But what happens when “just tired” starts to feel different? When fatigue lingers, shifts your mood or affects your daily routine, it may be your body’s way of asking for attention.
What “Feeling Off” Commonly Means
When patients say they feel “off,” they often describe symptoms like:
- Regularly feeling tired or drained
- Difficulty concentrating
- Changes in appetite
- Poor sleep
- Mild dizziness
- Mood changes, such as irritability or low motivation
Individually, these symptoms may not seem alarming. Together, or when they persist, they may point toward underlying issues such as anemia, thyroid imbalance, vitamin deficiencies, blood sugar changes, dehydration, stress-related conditions or early chronic disease.
The cause of fatigue in particular, can be tricky to identify. It is a common feeling virtually everyone experiences for a variety of normal reasons that have nothing to do with an illness. But it is also one of the most frequent early warning signs the body gives when something is not functioning optimally.
Duration vs. Intensity: When Time Matters More Than Severity
One of the most important factors in deciding whether to see a doctor is how long you’ve been feeling tired or drained.
A few days of fatigue after a busy week is normal. Two or three weeks of low energy without improvement deserves attention.
Even mild symptoms can signal something meaningful if they persist.
Ask yourself:
- Has this been going on for more than two weeks?
- Is it interfering with work, family life or daily responsibilities?
- Am I functioning below my usual baseline?
Intensity matters, but time often matters more. A severe, sudden symptom justifies visiting a health clinic or urgent care, but mild symptoms that linger quietly for weeks may also need evaluation.
Gradual Changes in Energy Levels vs. Sudden Shifts
Gradual changes often indicate conditions that build slowly, such as hormone imbalances, thyroid disorders, iron deficiency or chronic stress. You may not notice the shift at first. Instead, you gradually realize you are not feeling like yourself.
Sudden shifts, on the other hand, may signal infections, medication reactions, blood pressure changes or acute illness. If you feel a rapid and unexplained change in your energy, mood or physical state, it is important not to ignore it.
Sudden changes can feel alarming, but they are often linked to a specific cause that can be identified and addressed. Gradual, persistent changes in how you feel may take longer to evaluate and manage.
Tracking patterns can help your provider identify causes more quickly. Noting when symptoms began, how often they occur, and what seems to make them better or worse can provide valuable clues.
When to Monitor at Home vs. When to Schedule an Appointment
It is reasonable to monitor mild symptoms at home if:
- They are short-lived
- You recently experienced a clear trigger, such as travel or illness
- They improve with rest, hydration or stress reduction
However, you should schedule an appointment if:
- Symptoms last longer than two to three weeks
- You experience unexplained weight changes
- You notice frequent dizziness or lightheadedness
- Mood changes feel persistent or worsening
- Brain fog interferes with concentration or work performance
- Fatigue does not improve with adequate sleep
Trust your baseline. If something feels consistently different from your normal, it is worth checking.
How Primary Care Evaluates Vague Symptoms
One of the most important roles of primary care is evaluating nonspecific complaints. When you visit your provider for ongoing fatigue or feeling “off,” the evaluation often includes several steps.
Detailed Health History
Your provider will ask about:
- Sleep habits
- Diet and hydration
- Stress levels
- Work and home life
- Medication use
- Family history
- Recent life changes
Don’t leave anything out, because even small details can help narrow down possible causes. Candidness and honesty are recommended. Your primary care provider isn’t there to judge or embarrass you. Everything you say is held in strict confidence.
Medication Review
Certain medications, supplements or combinations can cause fatigue, dizziness or mood shifts. Reviewing your medications, supplements and use of drugs or alcohol can help your PCP narrow down potential causes.
Physical Examination
A routine physical exam can detect subtle signs of thyroid enlargement, anemia, dehydration, blood pressure abnormalities or other physical clues.
Lab Testing
Basic blood work is often ordered to check for:
- Iron levels and anemia
- Thyroid function
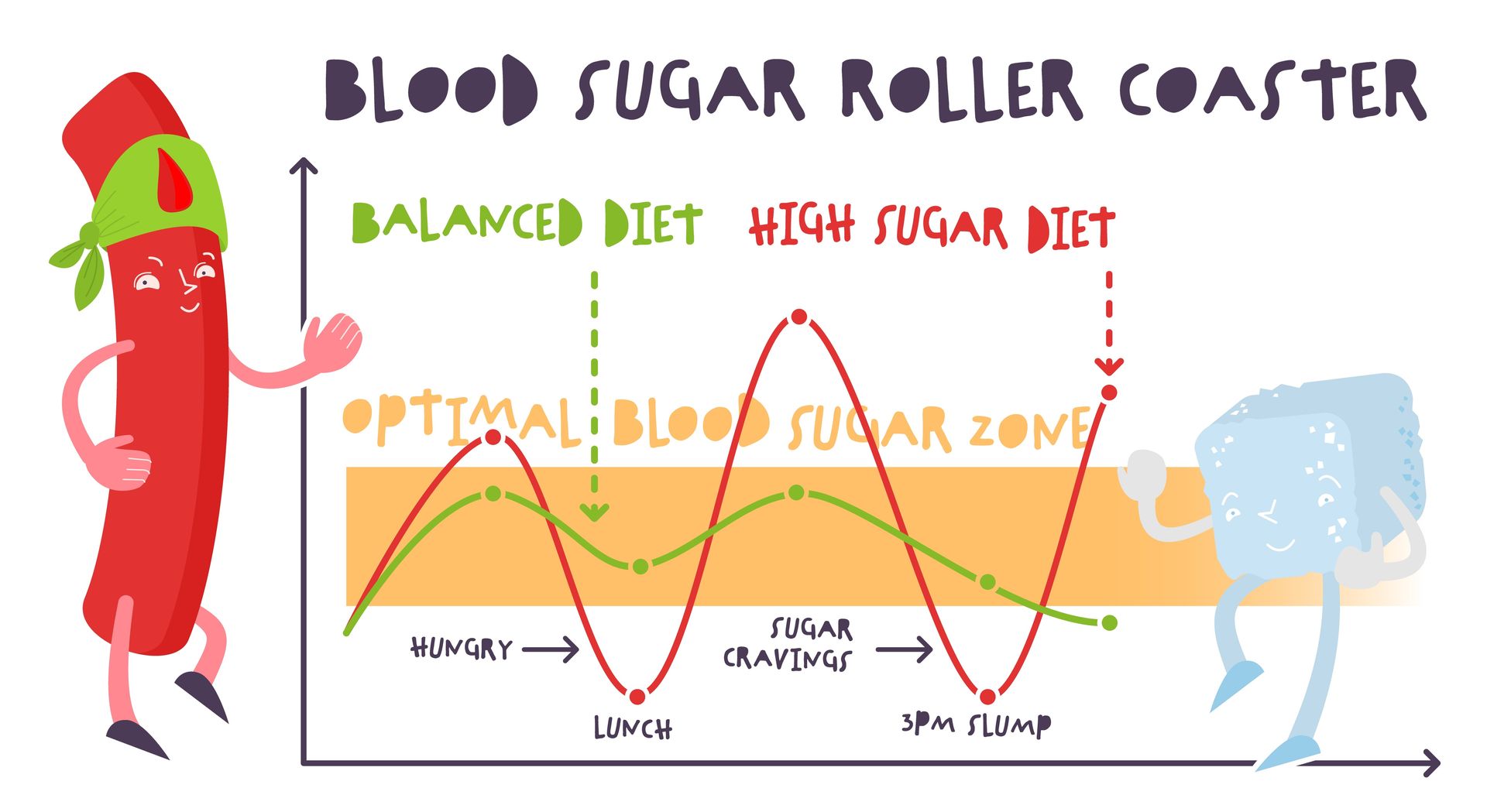
- Blood sugar levels
- Electrolytes
- Vitamin deficiencies
- Kidney and liver function
These tests provide objective data that can confirm or rule out common causes of fatigue and brain fog.
Screening for Mental Health
Chronic stress, anxiety and depression can present primarily as fatigue or cognitive fog rather than emotional symptoms. Screening tools help identify whether mental health support may be beneficial.
Why Early Evaluation Prevents Bigger Problems Later
Many chronic conditions begin quietly. Thyroid disorders, diabetes, autoimmune conditions and cardiovascular issues often develop gradually. Addressing symptoms early can prevent complications and reduce long-term health risks.
Early evaluation also brings peace of mind. If test results are normal, you can focus confidently on lifestyle adjustments rather than worrying about unknown causes.
Ignoring persistent fatigue can delay diagnosis and prolong unnecessary discomfort. Acting early allows for simpler, more effective interventions.
Comprehensive Primary Care at Our Healthcare Facility in Houston
If you have been feeling “just tired” but suspect something more may be going on, St. Hope Healthcare is here to help.
Contact us at (713) 778-1300 to schedule an appointment or visit one of our Houston-area health centers during clinic hours.